Patient Reported Outcome/Case Presentation
January 10 2024
Recently, the FDA has ceased accepting applications for approvals without patient-reported outcomes. This decision stems from the realization that 60 to 70% of research data, particularly in biology, cannot be reproduced. This alarming statistic indicates unethical practices among scientists and researchers, often resulting in manipulated outcomes. I have decided to adopt the practice of teaching through case presentations. In my case, it is not about scientists "cooking" outcomes; rather, it enhances the learning process.
By listening to patient-reported outcomes, we can learn how to effectively engage with patients during the initial evaluation. The upcoming case presentation will allow me to reassess my patient's condition. Before delving into my analysis and treatment plan, let's attentively listen to Gwynne's testimonial.
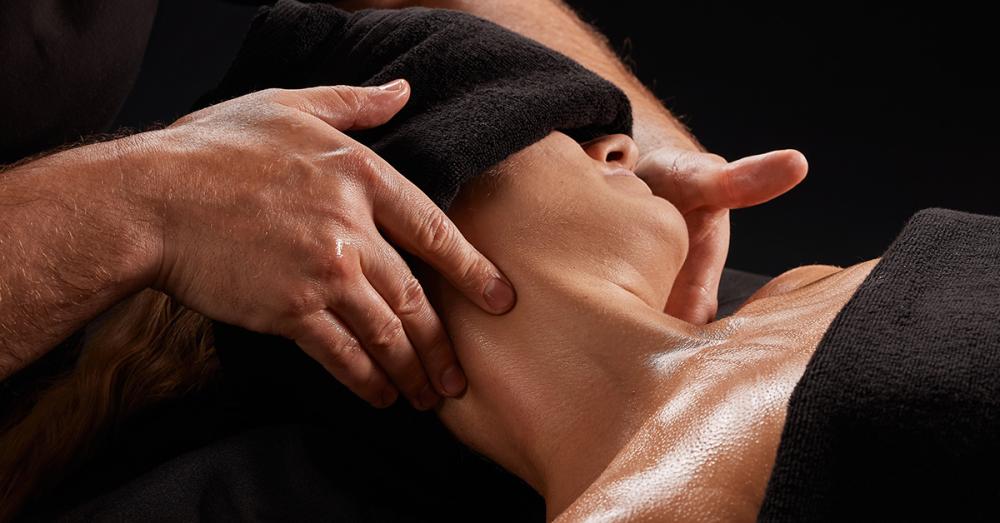
We understand that dizziness can result from various causes or combinations thereof. These causes remain unpredictable until we meticulously examine soft tissue, assess the autonomic nervous system through tests like dermographism, and more, tailored to each individual case. In Gwynne's case, I identified significant tension buildups in the neck and TMJ muscles. Could this tension be the cause of her disabling dizziness? Undoubtedly. The term "disabling" is not accidental; if a patient cannot drive due to dizziness, it qualifies as a disability.
Returning to my evaluation, I refrained from addressing and treating the neck and TMJ until performing the dermographism test, which revealed a notable autonomic irregularity. Subsequently, I examined the pulsation of the vertebral artery and couldn't feel it pulsating, suggesting tense muscles compromising the artery. Given the disabling symptoms, it became clear that the overly tense neck and TMJ muscles were responsible for the dizziness, with secondary vertebral artery syndrome and intracranial pressure contributing significantly. Focusing on all causes was essential for success in this clinically challenging case.
I decided to implement the protocol taught in program number 4 to address muscle/fascia tensions within the neck/TMJ, the techniques from program number 2 teaching how to check the pulsation of the vertebral artery as well as entire step-by-step protocols for vertebral artery syndrome, and the protocol from program number 15, where I teach the dermographism test and techniques to accelerate drainage of cerebral spinal fluid/eliminate intracranial pressure. A post-concussion protocol was also necessary for cases involving intracranial pressure/excessive cerebral spinal fluid accumulation.
Now, back to Gwynne's testimonial. I discharged her some time ago, highly recommending maintenance treatment every six weeks. At the time of discharge, I performed the dermographism test, which was good, and the range of motion within the neck and TMJ was normal. This suggested the normalization of resting muscular tone, and the pulsation of vertebral artery was sufficient. However, after watching her testimonial, where she reported driving but still experiencing some dizziness, I immediately contacted her and invited her back for evaluation.
I found that the soft tissue and range of motion were normal, the dermographism test was good, and the pulsation of the vertebral artery was normal. The episodes of dizziness without objective evidence led me to conclude that this is a sensitization phenomenon. I've provided three full-body stress management massages to address these memories. Please careful read body and mind chapter.
https://www.medicalmassage-edu.com/holism-vs-holistic-approach/
She now feels excellent, and in six weeks, she will return for maintenance treatment. This case is undoubtedly intriguing, and I welcome any questions or comments you may have.
Please post here Medical massage questions
Best wishes,
Boris Prilutsky
Add New
Comments
no comments found
Recents Posts





